Gestational Diabetes: What It Is, Risks, and How to Manage It
- Tazmin Lewis

- Jun 30, 2023
- 4 min read
Updated: Aug 27, 2025
Hello Mama/ Future Mama
Pregnancy is an exciting time, but for some, a diagnosis of gestational diabetes (GDM) can bring unexpected challenges. If you've recently been diagnosed or want to learn how to prevent it, you’re in the right place. As a specialist prenatal dietitian with years of experience in diabetes care, I’m here to guide you every step of the way.
What Is Gestational Diabetes?
Gestational diabetes is a type of diabetes diagnosed during pregnancy, typically around 26-28 weeks. It happens when your body can't produce enough insulin to keep blood sugar levels in check. It’s more common than you might think—affecting 10-20% pregnancies in the UK.
While some women have risk factors, GDM can happen to anyone—which is why screening is so important.
Who Is at Risk for Gestational Diabetes?
Some factors increase the likelihood of developing GDM, including:
Being over 40 years old
BMI over 30
Specific ethnic backgrounds (South Asian, African-Caribbean origin)
Family history of diabetes
Previous pregnancy with GDM
Having a baby over 10lbs (4.5kg) in a previous pregnancy
Although there are a number of risk factors as above, I have seen many women in my clinics without any risk factors too. Women with one or more or these will be offered a glucose tolerance test to check for gestational diabetes.
How Is Gestational Diabetes Diagnosed?
Most women are offered a Glucose Tolerance Test (GTT), which involves:
A fasting blood test
Drinking a 75g glucose drink
A second blood test 2 hours later
GDM is diagnosed if:
Fasting blood glucose is ≥5.6mmol/L
2-hour glucose reading is ≥7.8mmol/L
Some cases are diagnosed using an HbA1c blood test, but the GTT remains the most common method.
Why Does Gestational Diabetes Happen?
Raised glucose levels in GDM occur because the hormone insulin—which helps regulate blood sugar—isn't able to keep glucose levels within a normal range. Insulin is responsible for moving glucose from the bloodstream into the cells, where it can be used for energy or stored for later use.
During pregnancy, a newly formed organ, the placenta, produces several hormones, including progesterone and oestrogen. These hormones rise significantly as pregnancy progresses and contribute to insulin resistance—a condition where the body is producing insulin but struggles to use it effectively. As a result, glucose levels increase in the bloodstream.
Insulin resistance in pregnancy is a normal adaptation, ensuring that enough carbohydrates are available to support the growing baby. In women without GDM, the pancreas compensates by producing more insulin to keep blood sugar levels stable. However, in those who develop GDM, the pancreas is unable to keep up with the extra demand, leading to persistently high blood sugar levels.

What Are the Risks of Gestational Diabetes?
For Baby:
Macrosomia (large baby over 4kg)
Shoulder dystocia (baby’s shoulder getting stuck during delivery)
Premature birth (before 37 weeks)
Low blood sugar (hypoglycaemia) or jaundice after birth
Increased risk of Type 2 Diabetes later in life
For Mum:
Polyhydramnios (excess amniotic fluid)
Pre-eclampsia
Higher risk of future GDM or Type 2 Diabetes
Possible induction or C-section before the due date
Due to the above risks some women may be advised to have an induction or c-section before their due date. NICE guidance otherwise states to “advise women with uncomplicated gestational diabetes to give birth no later than 40 weeks plus 6 days. Offer elective birth by induced labour or (if indicated) by caesarean women to women who have not given birth by this time”.
To reduce these risks women are given target glucose levels and asked to check their blood glucose on waking (fasting) and also 1 hour after meals.
These targets vary across the country but NICE targets are:
Fasting <5.3mmik
1 hour post meal <7.8mmol
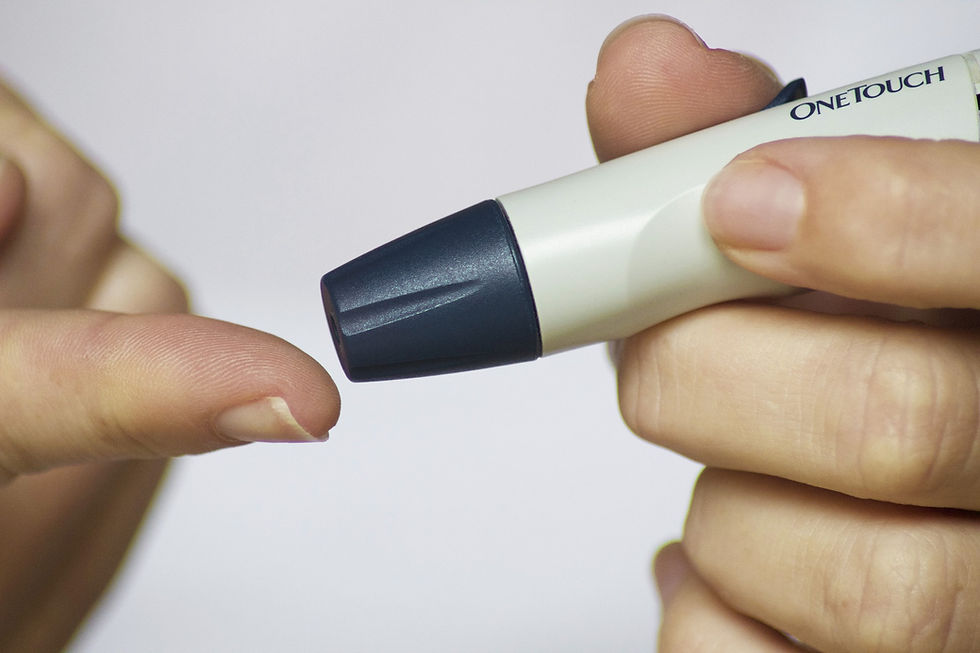
Managing Gestational Diabetes
The first-line treatment is making dietary changes and staying active. This includes: ✅ Eating a low glycaemic index (GI) diet
✅ Being mindful of portion sizes—especially carbs
✅ Incorporating regular movement (e.g. walking after meals)
For 1 in 3 women, diet and exercise alone aren’t enough, and they may need oral medications or insulin to keep blood sugar levels in range.
Example meal plan for gestational diabetes
Breakfast: 1-2 slices of seeded bread with 2 poached eggs, ½ avocado and mushrooms
Mid morning: Greek yoghurt with 5 strawberries and almonds, walnuts
Lunch: ½ plate quinoa, salmon and ½ plate side salad
Mid afternoon: 1-2 oat crackers with cream cheese, vegetable crudites
Dinner: ¼ plate brown basmati rice with stir fry chicken/tofu, broccoli, and peppers topped with sesame seeds
Evening/before bed snack: 1 medium apple with almond peanut butter
The key is to balance carbs with protein and healthy fats to stabilise blood sugar levels.
You’re Not Alone—Get Support Today!
Managing GDM can feel overwhelming, but you don’t have to do it alone. As a prenatal specialist dietitian, I’ve worked with countless women to help them manage their blood sugars with confidence.
💬 Want expert, personalised support? Get in touch today, and let’s create a plan tailored just for you!
Book a FREE discovery call today here
References
Plows JF, Stanley JL, Baker PN, Reynolds CM, Vickers MH. The Pathophysiology of Gestational Diabetes Mellitus. Int J Mol Sci. 2018 Oct 26;19(11):3342. doi: 10.3390/ijms19113342. PMID: 30373146; PMCID: PMC6274679.
Kampmann U, Knorr S, Fuglsang J, Ovesen P. Determinants of Maternal Insulin Resistance during Pregnancy: An Updated Overview. J Diabetes Res. 2019 Nov 19;2019:5320156. doi: 10.1155/2019/5320156. PMID: 31828161; PMCID: PMC6885766.




Comments